Also known as cranial nerve X or teeth cranial nerve, it is one of 12 pairs of cranial nerves extending from the various parts of the body, originating in the brain. This is the most complex and most protracted of the cranial nerves. The vagus controls many involuntary bodily functions, which are vital to the autonomic nervous system. It contains sensory and motor branches and fibers to numerous structures and organs. This includes the digestive system, glands, lungs, and the heart.
“Vagus” is a Latin term that means “wandering.” This accurately describes the extensive distribution of the nerve throughout the body. According to the National Library of Medicine, the embryology of the vagus nerve arises from the fourth branchial arch. This arch is responsible for developing organs such as the laryngeal cartilage, subclavian artery, pharyngeal and laryngeal muscles, and the aortic arch. In this blog post, we’ll discuss the functions of the vagus nerve, as well as its potential symptoms, diseases, and treatment.
Functions of the vagus nerve
Motor control of speech and swallowing

This is a critical function of the vagus nerve, as it plays a pivotal role in the intricate coordination required for these complex actions. The vagus nerve branches are known as the recurrent laryngeal nerve and the superior laryngeal nerve. These branches innervate the muscles involved in phonation, swallowing, and vocalization. The vagus nerve provides innervation to the larynx muscles in terms of speech, including the vocal cords and other intrinsic laryngeal muscles. The vagus nerve facilitates the relaxation of these muscles and their coordinated contraction, enabling us to form words and articulate sounds.
On the other hand, swallowing involves a complex series of muscle movements to propel liquids and foods to the esophagus from the mouth. In this process, the vagus nerve plays a crucial role by innervating the muscles involved in the pharyngeal and oral phases of swallowing. It helps coordinate the sequential contraction and relaxation of the muscles in the throat, upper esophagus, and tongue. This process prevents aspiration and allows for the safe passage of food.

Anti-inflammatory response

The vagus nerve has its involvement in inflammation regulation within the body. An excessive or uncontrolled inflammatory process can contribute to various conditions and diseases despite inflammation being a natural and immune response. The vagus nerve acts as a regulator of inflammation, which uniquely modulates this response. Anti-inflammatory effects are being exerted by the vagus nerve through a pathway called the cholinergic anti-inflammatory pathway.
Immune cells release cytokines or pro-inflammatory molecules when inflammation occurs. To counteract their effects, the vagus nerve detects the cytokines and initiates a feedback mechanism. The nerve releases acetylcholine, which are neurotransmitters that bind to specific receptors on immune cells, dampening the release and production of pro-inflammatory cytokines. The vagus nerve helps restore immune balance, promote tissue healing, and limit excessive inflammation.

Parasympathetic regulation

This plays a crucial role in maintaining overall balance and homeostasis within the body. The vagus nerve is responsible for promoting restoration, relaxation, and rest as a key component of the parasympathetic division of the autonomic nervous system. It’s important to note that the parasympathetic regulation works differently from the sympathetic nervous system, which is responsible for the “fight-or-flight” response of the body.
The vagus nerve stimulates the parasympathetic pathways when activated, decreasing blood pressure, heart rate, and respiratory rate. It helps to facilitate digestion, elimination, conserve and restore energy, and other vital processes necessary to maintain optimal physiological functioning. Vagus nerve activation initiates a cascade of physiological responses. For instance, the vagus nerve slows down the heart rate when it stimulates the heart, allowing it to beat more relaxedly.

Sensory information transmission
This function enables communication between different structures and organs in the brain and the body. This is a significant sensory pathway that relays important signals from the heart, digestive system, throat, lungs, and other visceral organs to the brain. The vagus nerve can provide sensory feedback about taste sensations from the back of the tongue and throat, helping to inform our perception of flavors and overall food palatability.
Furthermore, the vagus nerve provides valuable information about the internal environment of the body and monitors viral parameters. It relays signals related to oxygen and carbon dioxide levels, blood pressure, pH levels to the brain and chemical balance.

Conditions associated with the vagus nerve
Inflammatory bowel disease
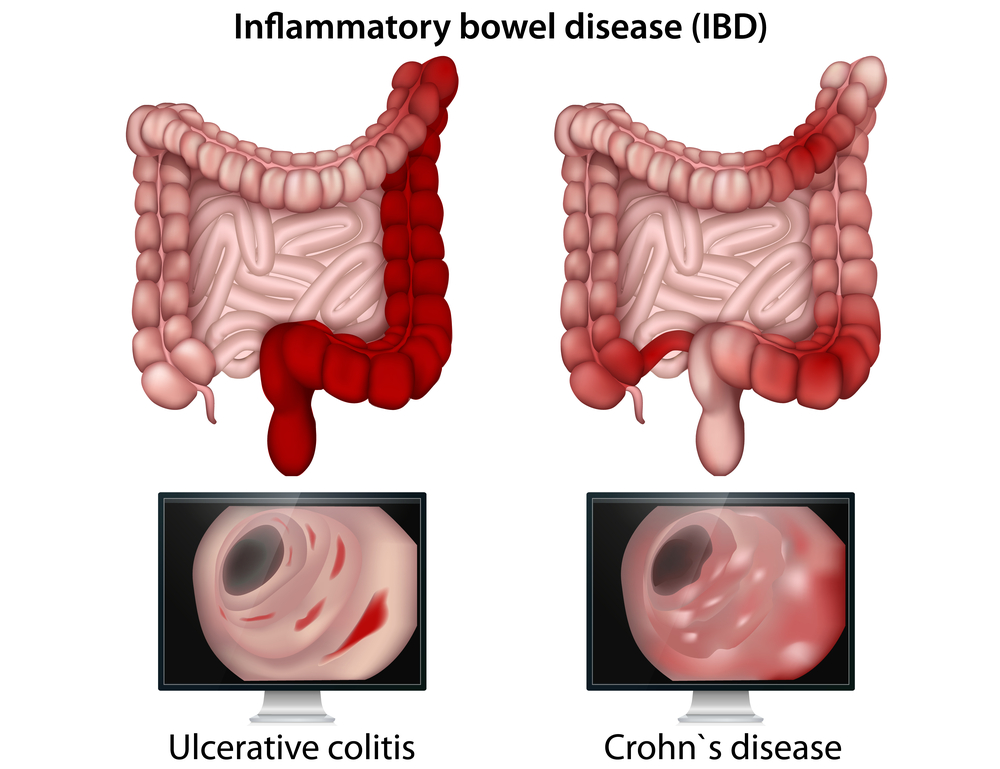
Inflammatory bowel disease (IBD) primarily encompasses ulcerative colitis and Crohn’s disease as it refers to chronic inflammatory conditions of the digestive tract. While the causes of IBD aren’t directly understood, they’re believed to have a combination of factors such as the environment, immune system, and genetics. The vagus nerve has been implicated in the regulation of immune responses and inflammation within the gastrointestinal system, which can impact the progression and development of IBD.
The vagus nerve can modulate the immune response through the cholinergic anti-inflammatory pathway and possesses anti-inflammatory properties as well. Reduced activity or dysfunction of the vagus nerve may be associated with a more severe cause of IBD and increased susceptibility to intestinal inflammation, according to some studies. The impact of impaired vagus nerve signaling can contribute to excessive inflammation within the gut and lead to immune system imbalances.

Gastroparesis
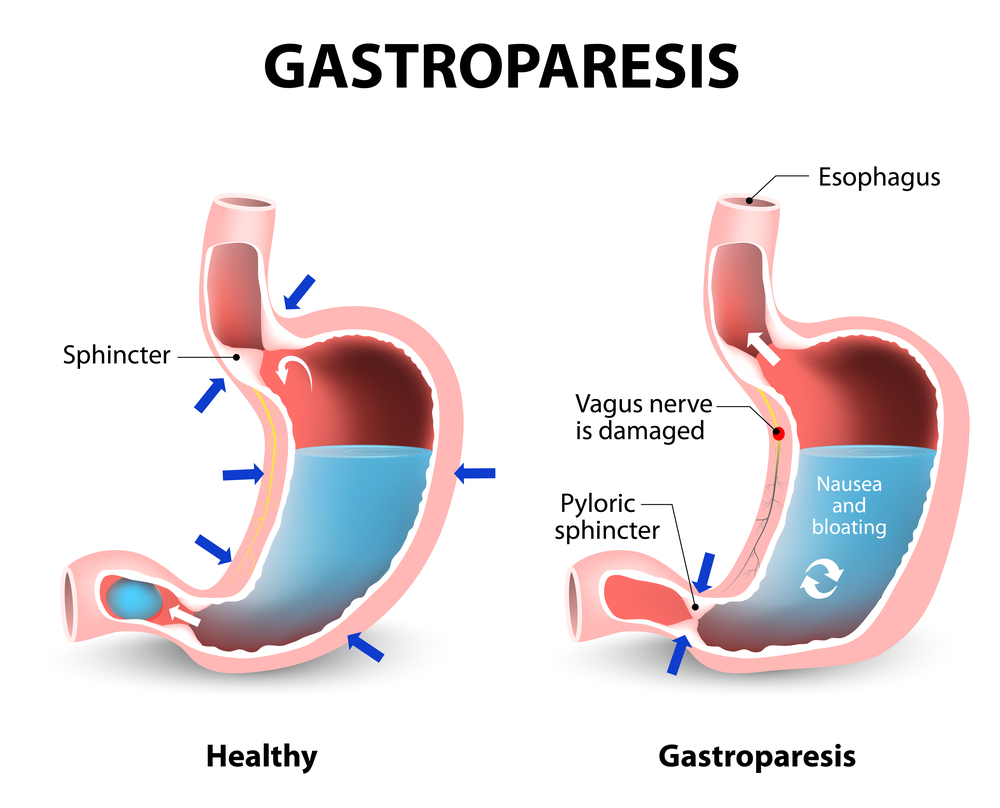
This is a condition that involves delayed stomach emptying due to dysfunctional or impaired motility of the stomach muscles. The vagus nerve plays a significant role in gastric motility regulation and can be engaged in gastroparesis development despite not exclusively being an illness of the vagus nerve. According to Cleveland Clinic, the vagal nerve damage associated with gastroparesis can result from viral infections, scleroderma, abdominal surgery, and diabetes.
Other potential causes may include certain medications, prior surgeries involving the vagus nerve or stomach, neurological conditions, viral infections, and autoimmune disorders. Disruptions in the coordination of the neural signals in the digestive system or abnormalities in the stomach muscles can also contribute to gastroparesis.

Vagal neuropathy
Also known as vagus nerve neuropathy, refers to the dysfunction or damage of the vagus nerve. It’s a condition that affects the normal functioning of the vagus nerve and can manifest in various ways depending on the extent and location of the nerve damage. Vagal neuropathy can occur due to several causes, such as trauma, surgery, infections, autoimmune disorders, and medical conditions. Trauma to the neck, abdomen, or chest can lead to neuropathy since it directly damages the vagus nerve.
On the other hand, certain heart surgeries and thyroid surgeries can inadvertently damage the vagus nerve. Even viral or bacterial infections can cause damage and inflammation to the vagus nerve. Neuropathy can be the effect of some autoimmune conditions like autoimmune autonomic ganglionopathy. Lastly, underlying medical conditions such as diabetes can also place risks to the vagus nerve. Symptoms of vagal neuropathy may include loss of gag reflex, difficulty swallowing, and changes in heart rate.

Depression and mood disorders

Vagus nerve plays a role in the regulation of mood and emotional well-being, despite not being the direct cause of depression or mood disorders. These complex conditions involve a combination of environmental, neurochemical, and genetic factors. The vagus nerve is often called the “rest and digest” system, a major component of the parasympathetic nervous system. It helps regulate different bodily functions such as digestion, respiratory rate, and heart rate.
The Vagus nerve can influence mood and emotional states through its interaction with the release of neurotransmitters and the autonomic nervous system, according to studies. Vagus nerve stimulation has been shown to intensify serotonin release and other neurotransmitters that play a role in mood regulation. Moreover, some studies indicated that individuals with reduced heart rate variability and impaired vagus nerve function may be more susceptible to depression and other mood disorders.

Treatments for the conditions associated with the vagus nerve
Treatments for inflammatory bowel disease (IBD)
It’s essential to keep in mind that instead of directly targeting the vagus nerve itself, the primary focus should be on managing the underlying inflammatory condition. You can start with taking various medications such as anti-inflammatory drugs (corticosteroids and mesalamine), biologic therapies (anti-tumor necrosis factor-alpha agents), and immunomodulators (methotrexate and azathioprine). These medications help reduce gut inflammation and target the immune system. On the other hand, it’s crucial to adopt a healthy lifestyle that includes avoiding trigger foods, regular exercise, a well-balanced diet, and stress management techniques.
Vagus nerve stimulation (NVS) can be a potential treatment for IBD. This involves the implantation of a device that sends electrical impulses to the vagus nerve, which aims to modulate immune responses and inflammation. In the aspect of mental health, you can seek support from mental health professionals such as counselors or therapists, which can be beneficial in managing stress, anxiety, and depression associated with the condition.

Treatments for gastroparesis

When you have gastroparesis associated with your vagus nerve, adjusting the diet is the first step and beneficial treatment. This may involve eating more frequent meals that are smaller and low in fiber and fat. Foods that are easier to digest, like pureed foods, soups, and well-cooked vegetables, can be recommended. Several medications, such as domperidone and metoclopramide, can improve stomach emptying.
Moreover, injections of botulinum toxin (Botox) may be recommended in some cases. This treatment involves Botox being injected into the pylorus (the opening between the stomach and small intestine) to improve gastric emptying and relax the muscle. Additional treatment would be gastric electrical stimulation (GES), where a device is implanted to deliver electrical stimulation to the pyloric balloon dilation or the stomach muscles. This involves stretching the pylorus to improve emptying.

Treatments for vagal neuropathy

Treatment will primarily involve addressing and managing the underlying condition if the neuropathy is secondary to an identifiable cause, such as infections, trauma, autoimmune disorders, and surgery. This may include appropriate medical interventions such as antibiotics, immunosuppressive medications, surgery, and other targeted therapies. Medications may also be beneficial as potential treatments for vagal neuropathy. For example, medications that target pain, such as autonomic dysfunction and gastrointestinal symptoms, may be considered.
Your doctor may also recommend occupational or physical therapy to improve overall functioning and help manage symptoms. These therapies can focus on exercises to enhance swallowing function, strengthen muscles, and improve coordination. Lastly, symptoms of vagal neuropathy, such as heart rhythm abnormalities, difficulty swallowing, and voice changes, would require specialized interventions. Voice rehabilitation techniques and speech therapy can assist with voice-related issues.

Treatments for depression and mood disorders

Cognitive-behavioral therapy (CBT), psychodynamic therapy, and interpersonal therapy (IPT) are examples of psychotherapy that can effectively treat depression and mood disorders. These therapies help individuals change and identify negative thought patterns, manage stress, develop healthy coping mechanisms, and improve interpersonal relationships. Psychotherapy can potentially affect vagal tone, even though it doesn’t directly target the vagus nerve.
On the other hand, antidepressant medications such as serotonin-norepinephrine reuptake inhibitors (SNRIs) and selective serotonin reuptake inhibitors (SSRIs) are usually prescribed to manage depression and mood disorders. They work by balancing brain chemicals associated with mood regulation, like norepinephrine and serotonin.